Itchy redness, short nights, endless creams: for many, eczema remains vague. This chronic inflammatory dermatosis affects between 10 and 20% of children and 4 to 5% of adults. And yet, what dermatologists see on a daily basis is often very different from popular belief.
In just a few years, biotherapies and targeted treatments have profoundly changed the management of atopic dermatitis. But what really matters in the eyes of specialists is how the disease manifests itself in you, what you do on a daily basis… and what you don’t always dare to say.
What eczema really hides behind the redness
To a dermatologist, eczema is not just “dry skin” or a single food allergy. It is a disease linked to genetic, immune and environmental factors, with very dry skin and a weakened barrier. It develops in outbreaks, but it is not contagious.
Professor Marie-Sylvie Doutre recalls that no single food or product has been identified as a major trigger for flare-ups; allergological assessments and elimination diets are therefore not systematic. On the other hand, doctors insist on gentle hygiene, cotton clothing and the daily use of emollients all over the body.
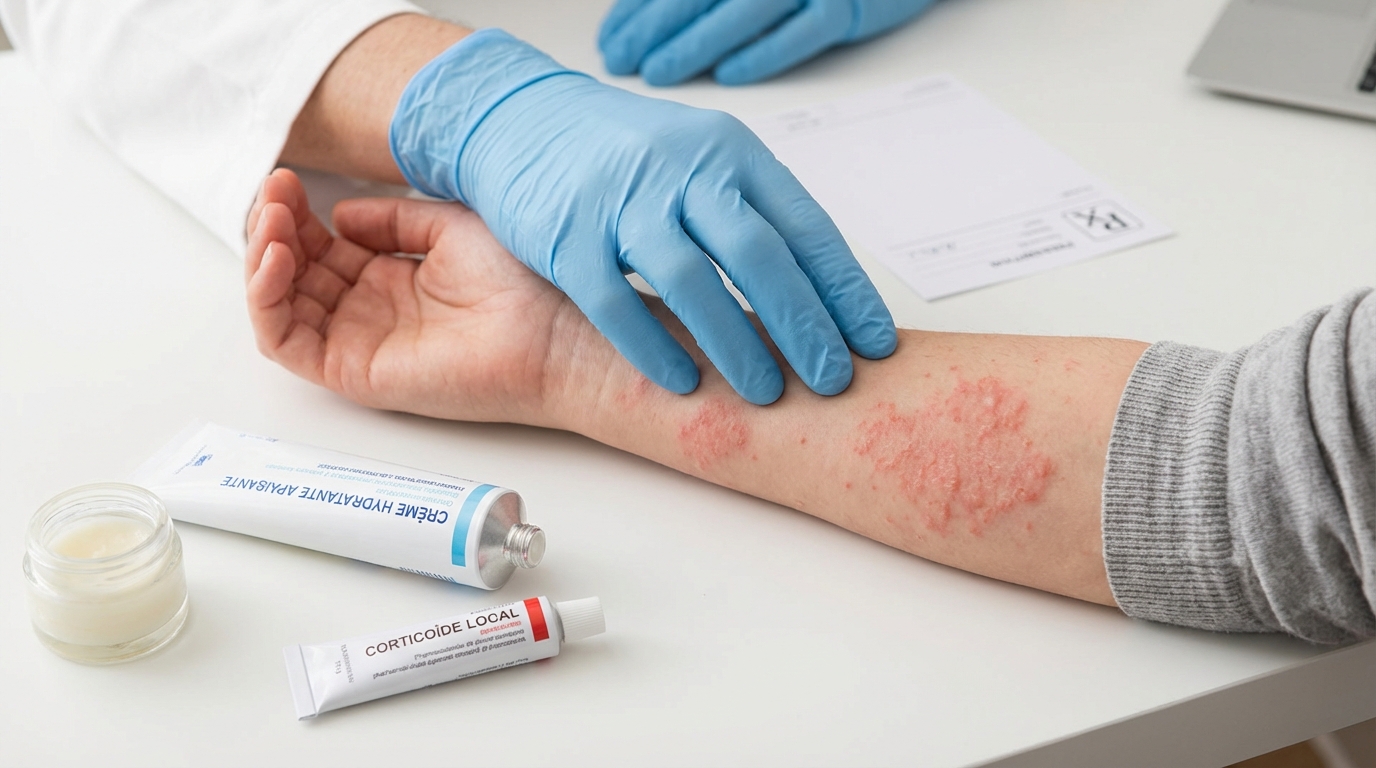
Eczema Treatments: What Dermatologists Really Do
First-line treatment of flare-ups is based on topical corticosteroids. On the body, French recommendations favor strong corticosteroids, once a day after a shower, until the lesions disappear; on the face, only moderate corticosteroids. Corticosteroid creams are applied to the plaques, moisturizers everywhere else.
When flare-ups are frequent, specialists switch to a proactive regimen: two days a week of corticosteroids or calcineurin inhibitors on the areas that usually flare. There remains observance. Professor Marie-Sylvie Doutre reports hearing patients say, or, she explains to . Used correctly, these local treatments control atopic dermatitis in approximately 85% of people.
Living with chronic eczema: what your dermatologist looks at
For 10 to 15% of patients, local care remains insufficient. The dermatologist then takes into account the severity of the lesions, the location (face, neck) and the quality of life, but also the quantity of corticosteroids used, for example more than four monthly tubes of 30 g of strong class in adults.
In these cases, general treatment can be offered, firstly cyclosporin after 16 years, for a limited period. Then come biotherapies by self-injections every two weeks and JAK inhibitors taken daily orally, prescribed in compliance with the 2023 ANSM recommendations. Any eczema lesion being colonized by Staphylococcus aureus, antibiotics are only given in the event of a real infection, and antihistamines only serve to help you sleep better for a few nights, while the lesions regress.
Is eczema contagious?
No, it is a chronic, non-contagious inflammatory disease.
Should allergy tests be done?
Not systematically, they are reserved for special cases.
When should you consider general treatment for eczema?
When local care fails and the disease remains severe.
